PHASE ONE: Repair/Acute post-op phase (immediate post-op to 1 week post op):
This is the initial days following surgery where the main goals of rehabilitation are to control pain and effusion and create an environment for early mobility within the surgical precautions. Basic modalities including the use of vasopneumatic devices can be very helpful in this phase for pain control. In addition, low grade mobilizations or simple long axis distraction can assist in pain control as well as decreased risk for adhesions.1 Basic exercises to facilitate activation of the lower extremity and stationary biking without resistance are typically initiated in this phase.
Common pitfalls of the repair phase include poor gait mechanics or avoidance of a foot flat gait progression. No matter what the procedure, patients should be encouraged to neutralize the ground reaction forces and ambulate with a normal heel to toe pattern to avoid over activation of the hip flexors during standing and walking. Even in the presence of microfracture, patients should be cautioned from holding the leg off the ground completely or utilizing a toe touch pattern. On the opposite end of the spectrum are patients who are overloading the surgical hip and therefore the healing tissues with too much or excessive weightbearing beyond the noted restrictions.
PHASE TWO: Rehab/recovery phase (3 to 7 days post op to 8 to 12 weeks post op):
In this phase there is a focus on restoring normal mobility, range of motion (progressing as the precautions are lifted), muscle activation, strength, and functional abilities within activities of daily living. It is crucial that normal arthrokinematics are restored in this phase when possible. In the case where the extent of the damage will not allow for this, it is important that all treating clinicians are aware of this and have a plan to work around any specific limitations. In addition, it is important as strength is restored in the musculature around the hip including the core, that the patient is able to control and manage loading in multiple functional positions such as quadruped, kneeling, and variable standing postures. Compensatory movement patterns should be identified and avoided during the progression of this phase.
Common pitfalls of the rehab/recovery phase include too soon or too much weight bearing activity beyond the patient’s muscular strength and endurance ability. Very commonly this phase results in one or two “honeymoon periods” where the patient is feeling very well and becomes overconfident in their abilities. If not careful, the athletic trainer may make this same mistake and progress the patient beyond what they are ready to handle. This can be combated with frequent assessment and re-assessment of strength and kinematics before, during, and after new or advanced activities are added to the rehab progression.
PHASE THREE: Reconditioning/return to training phase (12 to 20+ weeks post op):
This is the most variable and challenging phases of the post-operative rehab for athletes. In this phase the athlete should be working on skill development, force and load volume tolerance and management of recovery. Bridging the gap from the rehabilitation to the performance phase may take just a few weeks and upwards of a few months depending on the level of the athlete, the demands of the sport and position on the hip, and the procedures performed/damage identified intra-operatively. It is important that the athlete be well informed through the entire rehab process, but especially during this phase as the balance between workload and recovery will be a challenge if they do not assist in giving feedback on how they are feeling. Use of technology such as sleep and heart rate monitors, accelerometers, and motion capture systems can assist in the development of this phase when available. The athlete should not be experiencing any pain, loss of motion, or decrease in baseline strength as they progress in the reconditioning phase.
Common pitfalls in the reconditioning phase include premature advancement of stability and endurance challenges without appropriate movement patterns or trunk stability. In this phase commonly return to running may be a significant challenge if there is not appropriate muscular endurance, or if poor pre-surgery mechanics are not addressed. The use of video analysis by a trained member of the rehab team may be useful in combating some of these issues.
PHASE FOUR: Performance/return to play phase (16+ weeks post op):
This is the time from return to team practice through the end of the season and some would say until pre-season for the following season is completed. This is a variable process dependent on the specific sport and position. Ideally, if contact is involved, the player participates at his or her position taking reps at full speed with little to no contact and is gradually reintegrated into full return to unlimited play.
The two most common pitfalls as athletes return to play following hip arthroscopy are poor recovery planning/management and lack of adherence to a maintenance program as it relates to the strength and control of the muscles around the hip. The athletic trainer’s ability to keep these items in check as the player returns to sport is a critical aspect of successful return to sport.
MANY FACTORS IMPACT THE REHAB PROCESS
Rehabilitation following hip arthroscopy of an athlete can be a challenging task for the athletic trainer dependent on a variety of factors. Certainly, an athletic trainer is capable in their skills and abilities to follow the recommended protocols, however, very frequently these patients require extensive amounts of manual therapy interventions and one on one neuromuscular reeducation and strength progression that dependent on the athletic trainer’s setting, may not be realistic. For example, in a high school setting there may be one or two athletic trainers for the entire school handling all injuries across all sports. This is a very different set up than an NBA team with a multitude of medical staff and less than 15 athletes to care for.
It is not uncommon for athletes to be managed with a team approach following surgery, especially in the rehab and reconditioning phases. Typically, a physical therapist (PT) and athletic trainer (AT) team works very well for these athletes. The PT can manage the manual therapy needs as well as monitor the progression of motor control and strength development while the AT is able to spend more time in the progression of movement patterns and strength development.
Most importantly, when rehabilitating an athlete post hip arthroscopy, the key thing to remember is no one rehab progression is like the next. There are an incredible number of factors that go into the process and the entire rehab team as well as the athlete should be in constant communication regarding how the patient is progressing. Any setbacks along the way can typically be handled relatively easily when identified and addressed quickly.
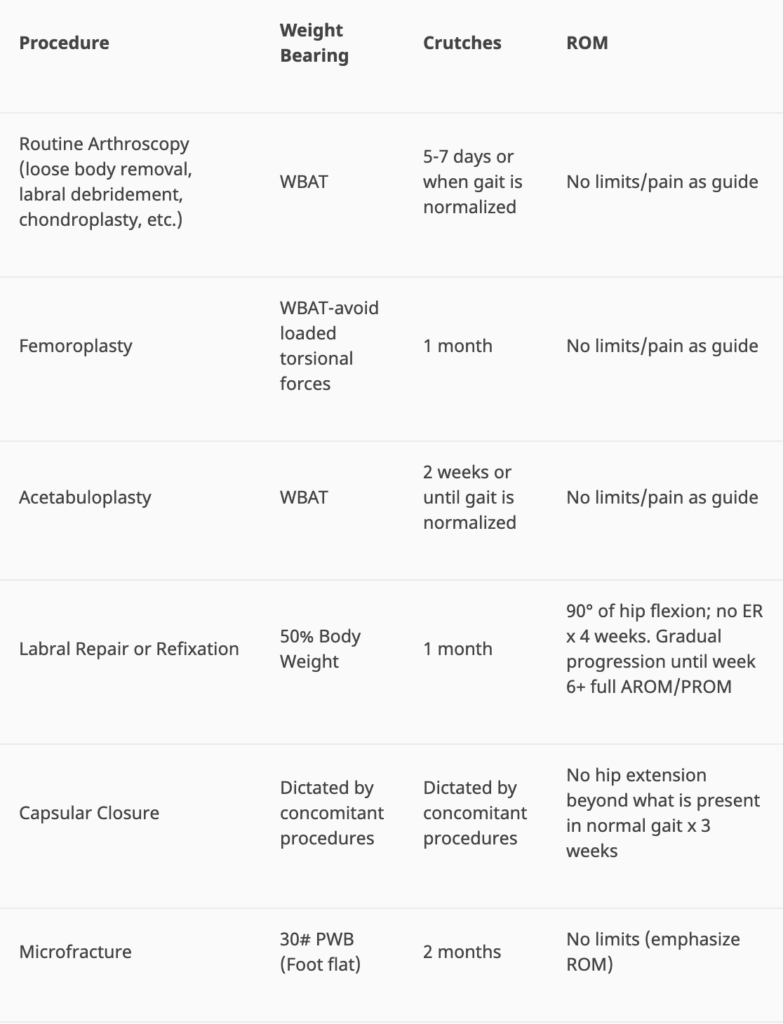
Basic weight bearing and range of motion restrictions for common hip arthroscopy procedures can be found in the following table:
Dr. Ashley Campbell with her Doctorate in Physical Therapy from Belmont University after completing her BS in Exercise Physiology at Ohio University. She is a Board-Certified Specialist in Sports Physical Therapy as well as a Registered International Sports Physical Therapist and Certified Strength and Conditioning Specialist. Ashley has spent her career working extensively in orthopedics and sports medicine with athletes at all levels including PGA, NFL, NBA, NHL, and MLB. She joined the Nashville Hip Institute team almost 5 years ago and since that time has assisted in growing and expanding the practice with her fellow clinicians including enhancements to patient care, research, and education for patients and other clinicians alike. Ashley lectures nationally and internationally on topics ranging from hip rehabilitation, to injury prevention and functional movement, including speaking at the International Society for Hip Arthroscopy annual meetings. She is a lead instructor with Advances in Clinical Education and holds an Adjunct Faculty position with Belmont University’s School of Physical Therapy in Orthopedics and Sports Medicine. She serves as an Associate Editor for the International Journal of Sports Physical Therapy and has won awards for leadership and clinical skills from Belmont University and the APTA’s Sports Physical Therapy Section. Most recently she received an award in at the International Society of Hip Arthroscopy meeting in Melbourne, Australia for her research related to arthrogenic muscular inhibition of the hip.
Dr. Michael Voight has been both an educator and clinical physical therapist for over 30 years. Presently, Dr. Voight is a tenured professor with Belmont University’s School of Physical Therapy in Nashville TN. He also holds a position of Adjunct Associate Professor in the Vanderbilt School of Medicine – Department of Orthopedics where he is the Co-Director of the Vanderbilt/Belmont Sports Physical Therapy Residency program. Dr. Voight has served as a Team Physical Therapist in the NFL and NBA. In addition, he has consulted with various teams in MLB, NHL and the MLS. He has worked at the Olympic Training Center, Olympic Festivals, Pan Am Games, Olympic Games, as well as with many noted golf PGA Tour Professionals. Dr. Voight maintains a clinical practice at the Nashville Hip Institute, specializing in orthopedic and sports related injuries particularly with PGA tour players, and serves on the advisory board of the Titleist Performance Institute. Dr. Voight has lectured extensively at various conferences, symposiums, and congresses both nationally and internationally having given over 900 professional presentations on a variety of orthopedic and sports medicine topics. Dr. Voight actively resides on the editorial boards of several different journals. He is currently the Editor-in-Chief of the International Journal of Sports Physical Therapy. Dr. Voight has won several professional awards, including the Distinguished Educator Award from the Sports Physical Therapy Section, the inaugural SPTS Lifetime Excellence in Education award, and the SPTS distinguished service award, Ron Peyton Award, and Presidents Award for his dedication to service. In 2010, Dr. Voight was selected into the SPTS Hall of Fame for a lifetime of excellence in sports physical therapy. His many accomplishments were again validated in 2011 when the American Physical Therapy Association presented Dr. Voight with their highest honor, naming him a Fellow of the APTA. In 2018, Dr. Voight was given the honor of being in the inaugural Titleist Performance Institute Hall of Fame for his achievements in the golf industry. Dr. Voight is an active member in numerous medical societies (AOSSM, ISHA, ESSKA, ISAKOS, ISHA) and was one of the founding members of the ICCUS Society. He remains extremely active in patient care, education, and research activities.
Reference:
- Willimon SC, et al. Intra-articular adhesions following hip arthroscopy: a risk factor analysis. Knee Surg Sports Traumatol Arthrosc. 2014;22(4):822-5.
Looking for more hip health? Don’t miss our article, “Hip Stretches to Boost Range of Motion.”
Request Program Information
Related Articles
Optimizing Athletic Performance: The Importance of Training Cycles According to Tom Zheng
In the world of athletic performance, training cycles play a [...]
Sleep: The Ultimate Recovery Tool You Need
In a recent webinar hosted by Concordia University Chicago faculty, [...]
Entry-Level Healthcare Administration Jobs
Entering the job market as a recent graduate with a [...]